Ring bone!
| July 8, 2013 | Posted by Melinda under Vet & Sports Medicine |
If you are enjoying these biology posts, I have a recommendation for you. I recently acquired a new textbook “Equine Exercise Physiology” by Hinchcliff and it’s fabulous!!!!!! Unfortunately it’s pricey and your library may or may not own it….but if you do enough leg work on the internet, you *might* be able to find a pdf version for free. I didn’t use the book specifically for this post, but I just read the chapters on tendons and ligaments and was very impressed, as they clearly explained the biology and current research without dumbing it down and gave specific training advice at the end of chapters. A huge point was made about how much adaptation and conditioning can really be done to different musculoskeletal tissues and their conclusion is that how a horse conditions is highly dependent on the work and conditioning that they did as yearlings and younger – ie being able to run around on pasture. The last paragraph of the tendon/ligament chapter gave me chills:
“After skeletal maturity, training will have no effect on tendon adaptation and therefore training should be directed at muscular, respiratory, and cardiovascu- lar fitness rather than the tendon.”
Instant sense of humility about any horse I’ve ever conditioned and took too much credit for their success or failure. Likely the fruits of my labor were sown well before the horse was even a thought in my brain.
But once again I find myself getting off topic!
Today’s post is based on a reader question.
Ring bone is a term used for osteoarthritis (OA) of the 3 lower joints of the horse’s leg. The bones are P1, P2, P3 (also called the proximal, middle, and distal phalanx among other names. The Distal phalanx/P3 is also called the coffin bone) and depending on which bones are involved you may hear the ringbone referred to as “high” or “low.
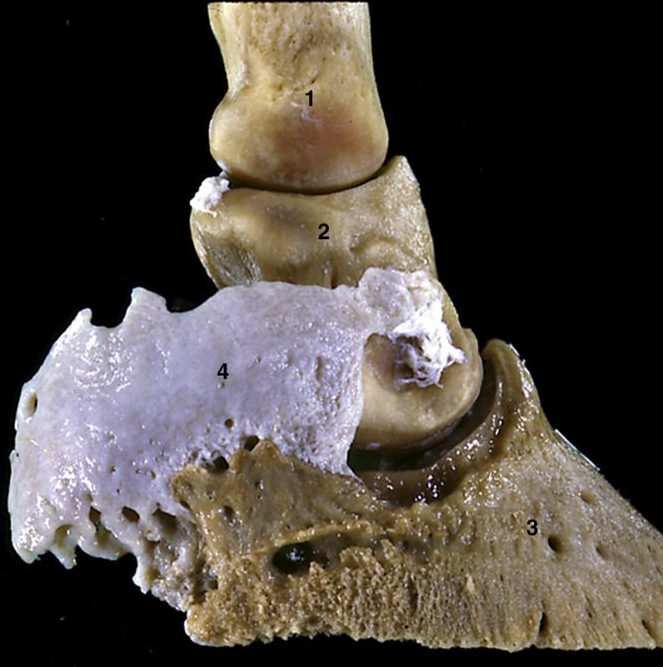
Picture Credits: Figure 23-21 Hoof cartilage attached to palmar process of distal phalanx. 1, 2, 3, Proximal, middle, and distal phalanges; 4, hoof cartilage.
(Dyce et al. Textbook of Veterinary Anatomy, 4th Edition. W.B. Saunders Company, 122009.)
Osteoarthritis is new bone is deposited (note that the “extra” stuff in the picture above is cartilage and is normal) around (periarticular) or in the joints (articular).
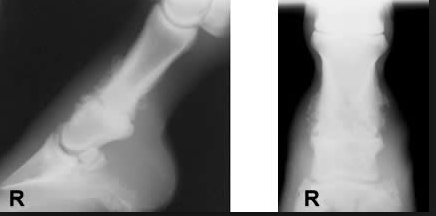
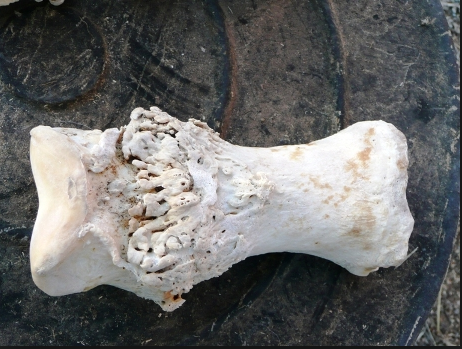
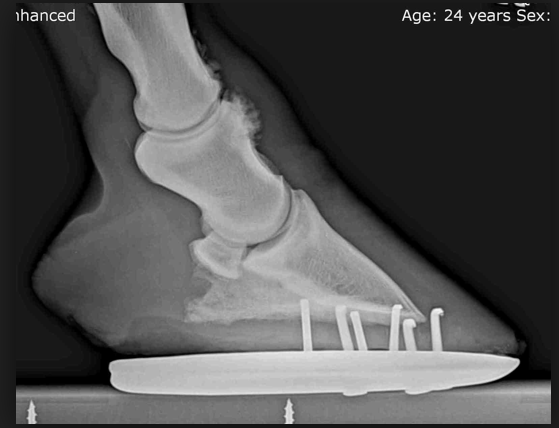
Here are some examples of ring bone (random pics from a google image search)
Nasty eh?
Now we get to the REALLY fun part. :). The WHY and the HOW.
In veterinary medicine there is a classification scheme called DAMNIT-V which classifies diseases according to categories like Degenerative, vascular, toxicity, etc. Working within this scheme does 2 things. When vets are considering possible diagnoses for a case (differential diagnosis, or DDx) using this acronomyn to think of possibilities from each category makes it less likely we will miss something.
The chart below is from dvm360.com (a website I regularly go to if I need vet concepts explained in simple language) that shows the DAMNIT-V (V = vascular and is sometimes not included) categories along with some examples.
So for a lame horse, there are many categories (and diseases) to consider. Is it inflammatory (osteoarthritis)? Trauma, mechanical, neoplasia (cancer), developmental (OCD)?
Based on signalment (age, breed, sex etc.), presentation, history etc. would make some diseases more likely than others. Diagnostics will further narrow it down.
Now let’s assume that indeed we have a case of osteoarthritis, which is a disorder whose mechanism of injury is inflammation.
Even at this simple first step (naming the disease and DAMNIT-V category) there is some controversy. Many of the internet resources list osteoarthritis (OA) as a degenerative disorder and even refer to it as “Degenerative Joint Disorder” (DJD). What I was taught in school is that OA, being a productive bony disorder whose basis is in inflammation, it is technically incorrect to refer to it as degenerative disorder and we were asked not to use DJD in describing it. Having not been in the real world clinics, I’m not sure what the general consensus is on this, so I will stick to what I was taught in class, and what is used in my favorite pathology book (Pathologic Basis of Veterinary Disease, 5th Ed, Zachary). So, for the basis of this discussion OA = inflammation.
It gets confusing because although OA occurred because of inflammation, as a joint disease it is classified as a noninflammatory joint disease. Inflammatory joint diseases are things like rheumatoid arthritis (which belongs in the immune-mediated DAMNIT-V category).
So, to summarize: Although OA is an inflammatory disorder, end stage OA is not an inflammatory joint disease.
Whew. Moving on.
Risk Factors for Developing OA
Zachary mentions that the number one risk factor for a human to develop OA is age (however this disease is NOT considered an inevitable consequence of aging) and most cases in humans are “primary”, meaning that there is no identifiable cause.
An example of a primary arthritis is me living to a ripe old age of…..I don’t know…..30? [I kid, I kid :)] and being told I now have arthritis and when I ask why, they say “it might be the running, or the riding, or the fact you broke your arm, or that fall down the stairs, or your bones line up funny or [insert your pet theory]……or a combination of living and that person next door who is your exact age and did the exactly the same things doesn’t have arthritis….so we really don’t know.
In animals most cases of arthritis seem to be secondary (ie – they have arthritis because of some other disease/injury/cause). (On a slightly related topic, the important predisposing factor – ie “primary” cause – for arthritis in animals is osteochondrosis – OCD).
Many different things can cause inflammation that lead to OA over time. Note that many of these factors are not specific to “ring bone” development but to OA development anywhere in the skeleton.
Here are some specific causes that I found among my sources:
-Traumatic injury – Wire injury to the pastern area that irritates/pisses off the periosteum of the bone. One concept pounded in my brain during this particular subject at school is that the periosteum has one response to being pissed off – make lots and lots of new bone.
-Abnormalities in conformation – long sloping pasterns, upright pasterns, long toe low heel, pigeon toed, splay foot. Conformation flaws can lead to excess strain or instability in one joint, causing inflammation.
-Joint instability (extra bone is deposited around joints that are instable in an attempt to stabalize it)
Joint surfaces that are incongruant
Inflammation of the synovium
Excessive joint strain because of a single misstep, or a repetitive overstrain leading to joint inflammation
An article at the Thehorse.com (which tends to be overall reliable source of information) cites “age, work, and concussive forces” as the three things that make a horse the most susceptible to ring bone. The article is citing Jeff Thomason, PhD, a specialist in equine biomechanics and anatomy at the Ontario Veterinary College at the University of Guelph and he goes on to say that ring bone tends to occur in older horses worked on hard surfaces much of their lives and acknowledges the horses at the most risk are those with long toes and low heels, and probably those horses with upright pasterns or high heels.
The original question that spawned this post was whether or not trotting over hard surfaces (like hard packed roads) was a risk factor in developing ring bone. I hope you are beginning to appreciate the difficulty in answering that question. First is the issue of “causality” which is proving something caused something else, especially when temporally separated as far apart as the work the horse might have performed, and the development of OA.
I’m not sure that the factors of “age, work, concussive forces” are very helpful when trying to tease out the cause of ring bone and make decisions in our training. Especially if the root cause is poor lower leg conformation. Age and work on poor conformation, especially over hard surfaces where more concussive force must be dispersed on an already poor structure is a plausible explanation, but doesn’t tell us whether a middle aged horse that has good conformation worked over moderately hard surfaces (like hard packed dirt roads) will later develop ring bone.
What’s my opinion?
Especially because other than possible association between poor conformation = potential joint instability/abnormal concussion absorption = inflammation = OA development, I’m not sold on increased concussive forces = OA.
Leaving aside traumatic injuries, it seems to me that the bulk of the evidence points to joint instability or other structural joint issues as the catalyst for this issue, and adding concussive forces, age, work etc. exacerbate the issue.
So, when I’m thinking about preventing ring bone and OA in general in my horses, I’ll spend more time looking and considering conformation than obsessing over the exact footing that I’m working over.
I think good structure and biomechanics + common sense/moderation of all footing types goes a long way to preventing these sorts of injuries. Too much of anything isn’t good. All sand training isn’t any better than all hardpacked dirt training. Doing all my training at a trot and never walking or cantering isn’t ideal either.
For a number of years my only available “every day” conditioning surface was extremely hard packed dirt road next to a canal, with some asphalt pavement interspersed. So, I did a lot of arena work to change up the footing. And a couple times a month I trailered out to an area that had a mix of different footing types.
Everything in moderation.
It’s also important to realize that a carriage horse being worked at a trot/jog over pavement is very different from what we are asking our endurance horses to do, even if our main conditioning trails are packed dirt roads and gravel. Ring bone and side bone is often cited as a “carriage horse” disease, even though it occurs in other breeds and disciplines.
In summary, ring bone and hard surfaces aren’t something I spend too much time obsessing about in my horses. I have a horse with good leg conformation, who is not a draft breed, who I try to work over a variety of surfaces, and chances are a career ending injury will be something other than OA development in the lower limbs. And even if ring bone is a significant factor in her life later on, it won’t necessarily be due to the ground we conditioned on – it’s more likely to be because of a pastern trauma injury (of which she has at least 2 healed scars, one which is much worse than the other) which are beyond my control, or because of an overtraining issue, or a “bad step” cause. And I’m equally as likely to injury her on ground that is too soft. In the herd of standardbreds that I work with for civil war reenacting, there are some horses that have ring bone and some horses that don’t. The horses all have a similar background and are managed in a very large pasture. While there is a wide variety of ages, much of the population is in it’s teens, with a substantial proportion in their 20’s or beyond. Some have it, some don’t. Some are symptomatic, some aren’t. Like many of the conditions that develop later in life, I think that we do not have the formula figured out for what exactly causes it, and while some of the risk factors might be known, there are a ton of confounding factors and there are other conditions that warrent our attention and perhaps our efforts at prevention. As with so many disorders and injuries, paying attention to conformation and structure can prevent so many issues!
OK – I think we’ve got the point: a wide range of factors that encompass everything from genetics and conformation to injury from overtraining/overstrain or “one bad step” can cause inflammation ==> OA.
But how does the inflammation lead to all that bone formation?
Inflammation is the short term protective response of the body to an insult or injury. The “hallmarks” of inflammation are “rubor, calor, tumor, and functio laesa”. Yes, I actually had to memorize that for a test. In simple english that translates to “redness, heat, swelling, and loss of function”. All of these things happen because of the innate immune system that has cells that respond to the insult/injury, and release cytokines/chemokines that are tiny molecules that act as chemical gradients to attract other “inflammatory” cells, and act on various biological entities such as cells, membranes, bone marrow etc to cause all the local and systemic effects that we associate with “inflammation”.
Acute inflammation is necessary and useful! This process that has us icing, taking NSAIDs, and elevating our poor sprained ankle are actually initiating the healing and repair process. However, an inflammation process that gets “too big” or goes on “too long” can cause excessive tissue damage. The inflammatory process can be a bit like the “shotgun” approach of the body to deal with something, rather than a finely honed needle. It’s an incredibly beautiful system that does an unbelievable job against a wide variety of insults…..but it’s also imperfect since it does have to deal with such a wide variety.
I’m purposefully glossing over much of the fine detail associated with the inflammatory response since it is a topic that really needs its own post if we are going to discuss, but in summary, all those little cytokines and chemokines are not only initiated the repair and healing process of the damaged tissue, they also affect the healthy tissues around the injury to some degree. And if that healthy tissue happens to be the perisoteum or bone, or the soft tissues intimately associated with the joint……that can lead to the instability, changes in the articular surface and everything else we have been discussing!
Ugh. Having spent WAY more time on this post than I should have today, it’s back into the lab to play with my bacteria and restreak plates!













It was a good opportunity for me to review some concepts that were taught two years ago! Its amazing how much I forget when it lies dormant in my brain. This was a fun post because I had never really thought about the root cause of ring bone and whether concussion really did create the condition. Knowing joint instability is the root of oa, and trying to relate that to concussion and realizing it goes back to confirmation was an ah ha moment. ! 🙂
Great explanation of ringbone! I’ve never had a horse get it and judging by those pictures am really thankful for that.
I’ll keep changing up what Cartman and I do each ride- and on what footing, so that we’re not out pounding on those hard packed roads every day!